Definition
- Eur J Obstet Gynecol Reprod Biol. 2011 Jun;156(2):131-6.
- Dtsch Arztebl Int. 2010 May;107(21):361-7.
Urinary tract infection (UTI) refers to a symptomatic bacterial infection within the urinary tract. This includes a lower urinary tract infection – cystitis (symptomatic infection of the bladder), or an upper urinary tract infection – acute pyelonephritis (symptomatic infection of the kidney). These definitions are based upon a grouping of symptoms. However, the bacterial infection may extend beyond the anatomical area suggested by the terminology.
Asymptomatic bacteriuria is present if a patient has two consecutive urine cultures showing >100 000 cfu/mL urine, but does not have any symptoms of a UTI. This is only treated in certain cases, such as prior to a urological operation, in pregnant women, or in immunocompromised patients.
UTIs may be considered complicated if symptoms of pyelonephritis emerge, or if a UTI is found in certain patient populations, including the immunosuppressed, men, pregnant women, diabetics, those with a history of pyelonephritis, or those with structural abnormalities of the urinary tract.
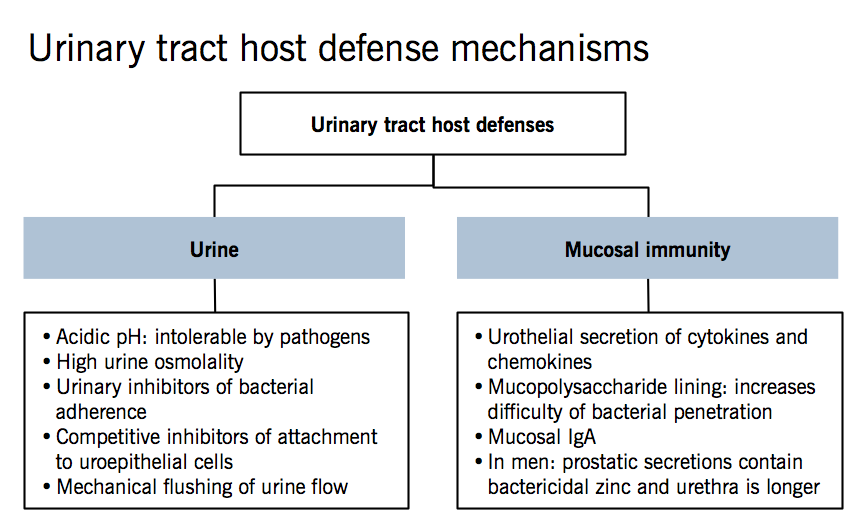
Urinary tract host defenses
- Infect Dis Clin North Am. 1987 Dec;1(4):751-72.
Except for the distal urethra, the urinary tract is normally sterile due to host defenses against bacterial colonization.
Etiology and risk factors
N Engl J Med. 2012 Mar 15;366(11):1028-37.
Lancet Infect Dis. 2004 Oct;4(10):631-5.
Etiology
- Most commonly due to infection with Escherichia coli species (80-90% of cases). Other causes include Klebsiella, Enterococcus, Proteus mirabilis and Staphylococcus saprophyticus.
- Periurethral colonization by the invading pathogen appears to be the initiating step in a cascade of events leading to a UTI.
- Most of the causative organisms are naturally present in the GI tract, which acts as a natural reservoir for potential UTIs.
Pathogenesis
- N Engl J Med. 2012 Mar 15;366(11):1028-37.
- Lancet Infect Dis. 2004 Oct;4(10):631-5.
- Radiographics. 2008 Jan-Feb;28(1):255-77; quiz 327-8.
Clinical presentation
- Eur J Obstet Gynecol Reprod Biol. 2011 Jun;156(2):131-6.
- Smith’s General Urology 17e, Chapter 3
- While UTIs may be classified in the literature according to location and symptoms, it is clinically very difficult to determine the extent of infection based on symptoms.
- Elderly women may present with only urinary incontinence and no other symptoms.
- Urine dipstick test showing positive nitrites or leukocyte esterase are suggestive of UTI, raising the pretest probability by 25%.
- Nitrite: positive due to bacterial reduction of endogenous nitrates to nitrites; classically positive in Gram-negative Enterobacteriaceae family of enteric uropathogens. However, nitrite dipstick may also be clinically useful in detecting Enterococcus and Staphylococcus bacteria.
- Leukocyte esterase: positive as neutrophil granules contain enzymes with esterase activity; presence of neutrophils in urine due to inflammation and leukocyte migration into the urinary tract.
- Only a positive urine culture is considered truly diagnostic of a UTI, however, urine should only be cultured in the setting of clinical infection or infective symptoms; as previously mentioned, asymptomatic bacteriuria is common and does not require treatment.
|
Symptom |
Corresponding sign |
Mechanism |
|
Dysuria |
|
Due to acute inflammation of the bladder, resulting in discomfort upon contraction during voiding. |
|
Frequency and urgency |
|
Reduced bladder capacity due to inflammatory edema causing decreased compliance and pain due to bladder distension. |
|
Hematuria |
|
Irritated, edematous urinary tract bleeding with voiding. |
|
Suprapubic tenderness |
|
Due to palpation and compression of an inflamed, edematous bladder. |
|
Chills and sweats |
Fever |
Inflammatory cascade resulting in a febrile response. |
|
Flank pain (may radiate to groin, often dull and constant) |
Costovertebral angle (CVA) tenderness |
Sudden renal edema, resulting in increased pressure and capsular distension. |
Treatment
- N Engl J Med. 2012 Mar 15;366(11):1028-37.
- Goodman and Gilman’s The Pharmacological basis of therapeutics 12e, Chapter 52
Treatment with antimicrobials aims to eradicate the bacteria causing infection. The chosen antimicrobials depend on extent of infection (uncomplicated or complicated), common local pathogens, and resistance patterns. Examples of antibiotics for uncomplicated UTI include:
- Trimethoprim-sulfamethoxazole
- Inhibition of microbial DNA synthesis by inhibiting the folic acid synthesis and consequently the purines required for DNA
- Fluoroquinolones
- Inhibition of microbial DNA synthesis by blocking DNA gyrase and topoisomerase IV needed for successful DNA replication and transcription.
- Nitrofurantoin
- The mechanism is not fully understood, but it directly causes selective damage to microbial DNA, which metabolises the toxic intermediates of nitrofurantoin more rapidly than human cells.