Overview/definition
Lancet. 2008 Jan 5;371(9606):64-74.
- Diseases of erythrocytes can be divided into the affected component of the cell as follows:
- Hemoglobin (e.g. sickle cell anemia, thalassemia)
- Membrane-cytoskeleton (e.g. hereditary spherocytosis); and
- Metabolism (e.g. G6PD deficiency)
- G6PD deficiency is a common, X-linked reduction in the activity of glucose-6-phosphate dehydrogenase (G6PD), which makes erythrocytes susceptible to oxidative stress and usually causes acute hemolytic anemia in response to a “trigger.”
- G6PD enzyme deficiency is the most common enzyme defect.
Etiology
Lancet. 2008 Jan 5;371(9606):64-74.
Am Fam Physician. 2005 Oct 1;72(7):1277-82.
IUBMB Life. 2012 May;64(5):362-9.
Am Fam Physician. 2005 Oct 1;72(7):1277-82.
IUBMB Life. 2012 May;64(5):362-9.
- G6PD gene is on the X chromosome:
- Males can be G6PD normal or deficient
- Females can be G6PD normal, intermediate (heterozygous) or deficient (homozygous)
- In heterozygous females, X-inactivation causes variability of G6PD activity from cell to cell and therefore variability in clinical presentation, especially if inactivation is skewed
- Around 140 mutations of G6PD gene are known and almost all are missense point mutations (one amino acid is changed in the G6PD protein from the wild type form, G6PD B)
- The mutations usually decreases stability of G6PD (results in less enzyme present) but can also acts qualitatively to change enzyme catalysis or substrate affinity
| WHO G6PD Deficiency Class | G6PD activity (% normal) | Phenotype |
| Class I | <10 | Chronic nonspherocytic hemolytic anemia |
| Class II | <10 | Intermittent hemolysis |
| Class III | 10-60 | |
| Class IV | 60-150 | Normal Activity |
| Class V | >150 |
- The two most common, polymorphic variants of G6PD deficiency are:
- G6PD Mediterranean (severe, Class II)
- G6PD A- (African descent, moderate, Class III)
- Chronic nonspherocytic hemolytic anemia (CNHA) is caused by a very small subset of the G6PD mutations which cause a more severe phenotype due to very low G6PD activity
- G6PD deficiency is most common in people of tropical and subtropical areas and there is support to show that this is due to a conferred resistance against Plasmodium falciparum infection, which causes malaria
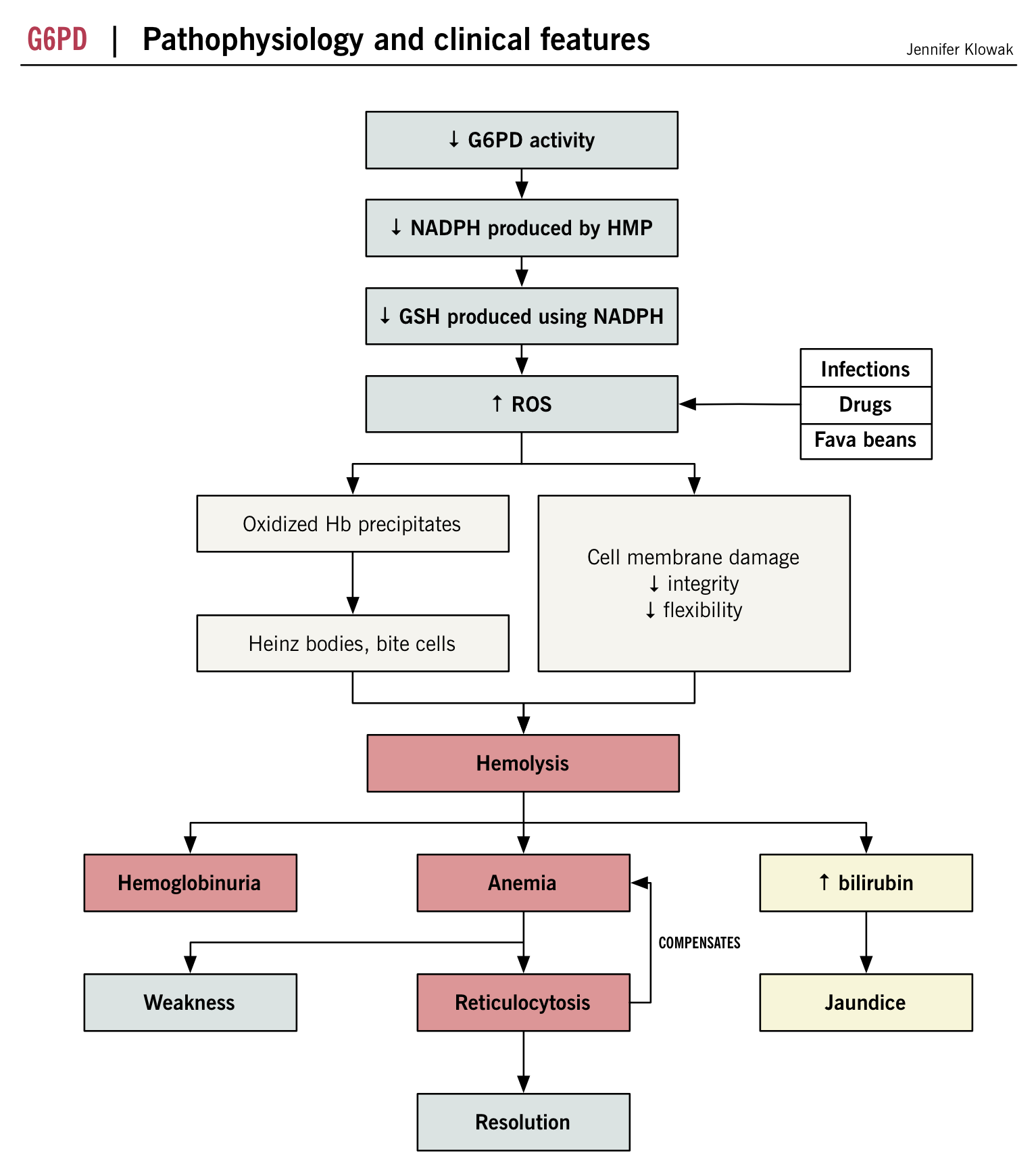
Physiology and pathophysiology
Voet Biochemistry pg. 862-867
Blood Rev. 2007 Sep;21(5):267-83.
Lancet. 2008 Jan 5;371(9606):64-74.
Blood. 1996 May 1;87(9):3953-8.
Current Paeds. 1995 Sep;5(3):190-4.
IUBMB Life. 2012 May;64(5):362-9.
Blood Rev. 2007 Sep;21(5):267-83.
Lancet. 2008 Jan 5;371(9606):64-74.
Blood. 1996 May 1;87(9):3953-8.
Current Paeds. 1995 Sep;5(3):190-4.
IUBMB Life. 2012 May;64(5):362-9.
Biochemistry of the pentose phosphate pathway (PPP)
- Glucose-6-phoshphate dehydrogenase (G6PD) is the enzyme for the first step of the pentose phosphate pathway (also called hexose monophosphate shunt or phosphogluconate pathway)
- G6PD reduces NADP to NADPH while oxidizing glucose-6-phosphate, which is the rate-limiting step of the pathway
- The pentose phosphate pathwayis a metabolic pathway which uses glucose-6-phosphate to produce:
- NADPH (most important)
- Phosphorylated sugars F6P and GAP; and
- CO2 and H+
| Important product of PPP | What it is | Product per glucose entering | Importance |
| NADPH (nicotinamide adenine dinucleotide phosphate) | An electron carrier, the reduced form of NADP+ | 2 NADPH / 1 glucose | Used by the cell for reductive reactions, protects against oxidation |
| Fructose-6-phosphate (F6P) | 6 carbon sugar with phosphate group | 2 F6P / 3 glucose | Continue using for energy or precursor for biosynthesis |
| Glyceraldehyde-3-phosphate (GAP) | 3 carbon sugar with phosphate group | 1 GAP / 3 glucose |
- For cells, ATP is considered an “energy currency” because the energy-releasing (exergonic) hydrolysis of ATP is coupled with endergonic (energy-consuming) reactions so that the reaction can proceed
- NADPH can also be considered an “energy currency” because it has reducing power which is used for reductive biosynthesis (making biomacromolecules such as fatty acids) and other reductive reactions (ex. reducing glutathione)
- Erythrocytes are especially vulnerable because the pentose phosphate pathway is their only source of NADPH.
Effect of decreased NADPH in the erythrocyte
- GSH (glutathione) is used to convert hydrogen peroxide and organic hydroperoxides (very reactive compounds) into stable compounds.
- NADPH is needed to regenerate GSH from GSSG (oxidized glutathione).
- Lack of GSH means GSH cannot protect the cell from the reactive oxygen species, which damage the cell membrane by oxidizing the protein and lipid constituents.
- As peroxides build up, cell membrane integrity and flexibility is reducedàhemolysis.
- NADPH also protects proteins such as hemoglobin from oxidation by protecting the sulphydryl goups.
- Heinz bodies (intracellular hemoglobin precipitates) form from oxidized, denatured hemoglobin which is no longer soluble.
Acute hemolytic anemia (AHA)
- Most G6PD deficiency patients are asymptomatic at baseline, but triggers can cause acute hemolytic anemia.
- There are 3 types of triggers:
- Fava beans: contain divicine, a strong oxidizing agent (compounds isouramil and convicine are also thought to increase PPP activity).
- Favism: AHA from consuming fava beans
- Infections: exact mechanism unknown, likely release of reactive oxygen species by the immune system.
- Drugs (some antimalarials, chemotherapeutic agents, sulfonamides, sulphones, antipyretics, analgesics, the diabetic agent glibenclamide, the gout treatment agent urate oxidase and miscellaneous).
- Whether the drug is a trigger can be dose-dependent.
- Mechanism depends on drug, for example production of ROS by liver during metabolism.
- Hemolysis then occurs because the formation of NADPH is insufficient for the oxidant stress.
- Erythrocytes are sensitive because the PPP is their only source of NADPH.
- Normally under stress, G6PD activity is increased to create sufficient NADPH, but a G6PD deficiency prevents this.
- Hemolysis results in anemia, which is usually normocytic and normochromic.
- Hemolysis is mostly intravascular.
- Patients usually return to normal because of compensation by increased erythrocyte production and/or removal of the oxidant stress.
- Reticulocyte count increases and usually causes resolution within 4-7 days.
- Newer erythrocytes can produce sufficient NADPH because they have a higher G6PD activity.
- A balance can develop between reduced life span of red blood cells under the oxidant stress and increased production of red blood cells.
- The anemia may not be self-limiting in severe cases and the development of acute renal failure from ischemia or haemoglobin casts is a rare complication.
Chronic nonspherocytic hemolytic anemia (CNHA)
- G6PD deficiency can, when more severe, be a cause of chronic nonspherocytic hemolytic anemia.
- Spherocyte = small, hyperchromic and circular erythrocyte
- The hemolysis is mostly extravascular in CNHA.
- Characterized by chronic anemia, usually with compensatory reticulocytosis but can be transfusion dependent.
- CNHA is anemia without a precipitating cause but hemolysis can be exacerbated by oxidative stress.
Clinical features
- Most patients are asymptomatic and not anemic throughout their life, but triggers can cause acute hemolytic anemia usually after a couple days.
- There is an increased risk of neonatal jaundice. The cause is more likely associated with a decrease in the G6PD-deficient-liver’s conjugation and clearance of bilirubin rather than an increase in hemolysis.
Clinical features of an acute hemolytic anemia episode
| Symptom | Sign/lab finding | Mechanism |
| Weakness/fatigue | Anemia | Hemolysis |
| Jaundice | Accumulation of unconjugated bilirubin | |
| Splenomegaly | Not usually expected, consider coexisting disease | |
| Dark urine | Hemoglobinuria | Hemolysis resulting in hemoglobin filtering into the urine |
| Low or absent haptoglobin | Haptoglobin binds hemoglobin after hemolysis and the complex is cleared from circulation | |
| High LDH | LDH is an intravascular enzyme released from erythrocytes during hemolysis | |
| Heinz bodies: circular inclusions inside red cells | Form from precipitated hemoglobin due to oxidation and denaturation. | |
| Bite cells: red cells with ‘bites’ taken out | ‘Bites’ are from splenic macrophages removing the part of the red blood cell with a Heinz body. | |
| Blister cells: red cells with a clearing at the periphery, like a blister | Arises when bite cells undergo repair of the cell membrane, resulting in a clearing within the red cell where the Heinz body previous was. | |
| Anisocytosis: unequal red cells sizes as indicated by increased red cell distribution width (RDW) | Hemolysis leads to increased cell fragments. | |
| Polychromasia: immature red cells on peripheral smear | Hemolysis leads to increased reticulocytes. Immature red cells have a grey-blue tinge, and this difference in colour is referred to as polychromasia. |
- Chronic nonspherocytic hemolytic anemia due to G6PD deficiency presents with:
- Neonatal jaundice,
- An enlarged spleen; and
- Increased chance of gallstones (bilirubin stones due to increased bilirubin from heme breakdown).
Diagnosis
- Diagnosis by fluorescent spot test or quantitative spectrophotometric assay, which measure G6PD activity its ability to form NADPH.
- G6PD activity can be falsely normal in acute hemolytic anemia because:
- (1) G6PD activity is higher in newer red blood cells, which now make up a greater proportion of total erythrocytes; and
- (2) a heterozygous female’s red blood cells with low G6PD activity will be destroyed preferentially and can even give a normal result in steady-state
- Provisional diagnosis upon blood smear (which can be obtained quickly) and consideration of patient’s origin and presentation.
Treatment
- Most hemolytic episodes are shortlived. Treatment is aimed at preventing acute hemolysis, mainly by avoiding triggers.
- Blood transfusion if severe.
- Possible future gene therapy or free-radical scavenging drugs.